I recently did a post about the first U.S. patient to undergo deep brain stimulation via implant, with the intent of interrupting a very stubborn pattern of opioid use. I didn’t want to pass up a chance to a closer look at that first case, however.
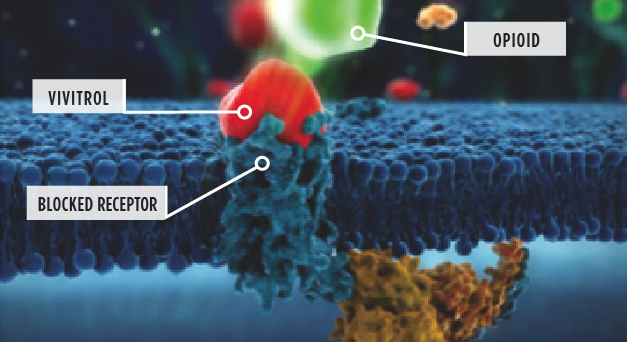
Deep brain stimulation is being tested to treat opioid addiction
The patient was 33 years old at the time of the surgery. Relatively young, in other words. He presented with a history of having been “unable to remain sober for more than four months since the age of 15, despite trying a variety of medications and other inpatient and outpatient treatments.”
That in itself is not terribly unusual. Certainly not for opioid patients; four consecutive months clean is actually better than many I’ve encountered over the years. Opioids are stubbornly addictive, create strong physical dependence, and are characterized by persistent drug hunger that undermines attempts at long-term recovery.That’s why so many wind up choosing Opioid Maintenance Therapy (OMT) over drug-free programs. They’ve tried other paths but failed, often many times over.
And not infrequently, continue to struggle even on high maintenance doses of methadone et al.
I recall one patient who arrived in inpatient rehab following a dozen failed hospital detox admissions. He was angry with his family because in his mind, he had been making excellent progress on his own (his family strongly disagreed). “They just don’t understand,” he argued passionately. “I was clean for, like, two whole months.” That was a personal record, see?
Our surgery patient describes his first experience with opioids in the aftermath of shoulder surgery at age 15 – the result of a football injury. Looking back, he’s convinced he was hooked in a matter of days.
Now that’s a story many of us will have heard before. It’s clear from research that genetics plays a role in determining who gets addicted and how severe that addiction is. Environment also has an impact, and the relative contribution of genes and environment can vary quite a bit between individuals.
That’s true for alcoholism as well. One psychologist observed that most of the patients he treated for alcoholism were able to describe, often vividly, their initial experience with alcohol. That wasn’t true for the rest of his patients.
It’s also possible that for some, opioids just push a pleasure button in the brain that makes the experience far more memorable than for most patients. It’s not something they would know about, until it happened.
“I fell in love with the feeling that gave me within the first couple days. I instantly knew this medication was something I was going to have to have.” Nothing ambivalent about that reaction.
If problems do develop during the first couple years of substance use, as they often do, they’re intermittent, easy to explain away. It’s only as problems worsen over time that the user gradually begins to question drug use.
He goes on to admit he “…soon turned to heroin, lost a football scholarship and has struggled with addiction ever since. Without drugs, he said, he is unable to feel joy or pleasure.”
That’s generally characterized as a form of anhedonia, often found among patients with depressive disorders. Over time, activities that once brought joy or pleasure no longer do so, at least to the degree they once did. That further contributes to social withdrawal and growing isolation.
As often happens, even heroin lost its allure. Without the pleasure it once provided, addiction was largely a matter of staving off the pain and discomfort of withdrawal. That required considerable quantities of drugs, and meeting the need for drugs consumed much of his time and energy. Growing anxious, he added Xanax to his daily regimen.
By that point, he was motivated to quit drugs, but lacked the ability. Multiple failed attempts at getting clean were short-lived, leading to another failure. The hunger for drugs overcame whatever resolutions he would make. It didn’t take long.
Worth noting that benzodiazepine can also induce physical dependence, and benzo withdrawal can be even more difficult to tolerate than heroin. I’m not sure why anyone would prescribe sedatives for someone with a substance abuse history like this patient had, but I doubt it’s all that uncommon.
It could be he concealed or minimized that history, as often happens.
He goes on to say that after “…numerous stays in long-term treatment, numerous detoxes. You name it, I’ve had it…” — he was ready for something radical.
I give him credit for his efforts to quit, even the unsuccessful ones. At least he kept trying. Many would simply have given up.
Still, invasive brain surgery is as radical a solution as I’ve encountered. It’s clearly not the answer for every opioid addicted individual. The risks that go along with surgery go up with advancing age and declining health, and this man, a former star athlete still in his early 30’s, might well have been a far better candidate for surgery than many others.
Also, he’s yet to reach two years opioid-free. I’ve known people who’ve relapsed after far longer periods in recovery.
There’s so much more we have yet to learn.