Aging in Recovery
She emphasizes how much stigma is encountered by older recovering persons in the healthcare system.

Select Page
by C. Scott McMillin | Feb 6, 2025 | Recovery | 0 |
She emphasizes how much stigma is encountered by older recovering persons in the healthcare system.

by C. Scott McMillin | Oct 20, 2022 | Addictive Substances, In the News | 0 |

by C. Scott McMillin | Sep 8, 2022 | Addiction | 0 |

by C. Scott McMillin | Jan 20, 2022 | Addiction Clinicians, People in Recovery | 0 |
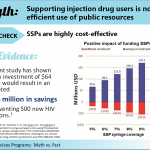
by C. Scott McMillin | Jul 8, 2021 | Public Policy, Resources | 0 |

by C. Scott McMillin | Apr 1, 2021 | Public Policy | 0 |
by C. Scott McMillin | Mar 25, 2021 | Addiction | 0 |
“Now, whether I have one drink or 10,” she admits, “I know I’ll still be where I started, in the nook of my sofa with the TV on at half-volume, anxiously biting hangnails.”
Read Moreby C. Scott McMillin | Feb 18, 2021 | Programs | 0 |
Logically, the disease model of addiction shouldn’t threaten anyone’s belief in their own ability to recover, any more than a diagnosis of diabetes or hypertension suggests you can’t successfully recover from those illnesses.
Read Moreby C. Scott McMillin | Dec 12, 2019 | Thinking About Addiction | 0 |
There’s a lot of laughter in the recovery world, mostly at oneself. Believe me, it helps.
Read Moreby C. Scott McMillin | Oct 3, 2019 | Programs | 0 |
These volunteers work for the welfare of the community by supporting the important work of your organization.
Read Moreby C. Scott McMillin | Sep 26, 2019 | Addiction, Thinking About Addiction | 0 |
“He’s a drug addict,” we’ll hear someone say. “You know what those people are like.”
Read Moreby C. Scott McMillin | May 24, 2018 | Public Policy | 0 |
Nonetheless, in most instances it’s an a priori resistance rooted in fear, rather than legitimate objections.
Read Moreby C. Scott McMillin | Mar 19, 2018 | Thinking About Addiction | 0 |
Too many doctors worry about “those people” showing up in the waiting room. They don’t particularly want to be known as a resource for the addicted.
Read Moreby C. Scott McMillin | Nov 23, 2017 | People in Recovery | 0 |
…struggles can actually serve as a disincentive to someone who knows you and is now beginning to peer uncertainly up their own long and bumpy road of life change.
Read Moreby C. Scott McMillin | Nov 6, 2017 | Addiction, Public Policy | 1 |
…healthcare advocates have to work extra hard while proponents of a more punitive approach simply point to a crime committed by a drug user…
Read Moreby C. Scott McMillin | Oct 19, 2017 | Addiction, Thinking About Addiction | 2 |
Nurses and doctors experience the same feelings about homeless alcoholics they see in the ER every Saturday night.
Read Moreby C. Scott McMillin | Oct 2, 2017 | Public Policy | 1 |
I fear they’re regular Americans, like some of us, except for their twisted attitudes and beliefs about addiction.
Read Moreby C. Scott McMillin | Sep 4, 2017 | Public Policy | 0 |
When you’re addicted, it’s probably more correct to say that your addiction is abusing you. And will continue to do so if allowed.
Read More