Fool Me, Please
...a chatbot doesn’t actually feel anything for the user. It’s simply doing what it was programmed to do. Principally, that’s serving as a perfect mirror.

Select Page
by C. Scott McMillin | May 25, 2026 | In the News | 0 |
...a chatbot doesn’t actually feel anything for the user. It’s simply doing what it was programmed to do. Principally, that’s serving as a perfect mirror.

by C. Scott McMillin | Apr 6, 2026 | Addiction Clinicians | 0 |

by C. Scott McMillin | Jan 29, 2026 | Resources | 0 |
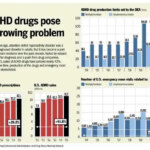
by C. Scott McMillin | Sep 1, 2025 | Addiction Clinicians | 0 |

by C. Scott McMillin | Jul 7, 2025 | Addiction Clinicians | 0 |

by C. Scott McMillin | Mar 3, 2025 | Treatment | 0 |
by C. Scott McMillin | Feb 17, 2025 | Addictive Substances | 0 |
What is it about having consumed hallucinogenic tea in a remote forest clearing, and as a result, spending the next few hours first vomiting, then hallucinating, and finally alternating between euphoria and intense fear, that could possibly transform the user into better, more effective corporate leader?
Read Moreby C. Scott McMillin | Jan 27, 2025 | Addictive Substances | 1 |
A whole range of psychedelic substances can apparently trigger HPPD
Read Moreby C. Scott McMillin | Dec 9, 2024 | Addiction Clinicians | 0 |
“somewhere between 45% and 70%…who have a diagnosis of bipolar disorder will have at some point in their lifetime met the criteria for a substance use disorder.”
Read Moreby C. Scott McMillin | Jul 15, 2024 | Addiction Clinicians | 0 |
In the past, the task of selecting the right treatment for a depressed patient has been more than a little hit or miss, involving a certain amount of trial and error.
Read Moreby C. Scott McMillin | Jun 3, 2024 | Addiction Clinicians | 0 |
One criminologist I met characterized ASPD as a “job description for a life of crime… especially the sort where you keep getting caught.”
Read Moreby C. Scott McMillin | Oct 23, 2023 | Addiction | 0 |
From a counseling perspective, it was clear to our clinical team that his habitual Internet use had reached a point where it was inseparable from his drug use.
Read Moreby C. Scott McMillin | Oct 17, 2022 | Addiction Clinicians | 0 |
The term was invented in the 1930’s to describe someone prone to becoming psychotic or severely disturbed under stress, but who otherwise was capable of functioning normally.
Read Moreby C. Scott McMillin | Aug 11, 2022 | Thinking About Addiction | 0 |
…so long as no claim is made for the product as a treatment or cure for a specific disease or condition, then “they can say anything they want to” about the supposed benefits of using it.
Read Moreby C. Scott McMillin | Jun 9, 2022 | People in Recovery | 0 |
These episodes occur “out of the blue,” not in conjunction with a known fear or stressor.”
Read Moreby C. Scott McMillin | Jun 6, 2022 | Addictive Substances | 0 |
The less good news, if I can call it that, is that none of the three was found to be more effective than our old friend, placebo.
Read Moreby C. Scott McMillin | Mar 24, 2022 | Addiction Clinicians | 0 |
…treat the two as independent and coequal in the clinical picture. Address them via an integrated treatment plan.
Read Moreby C. Scott McMillin | Mar 17, 2022 | Addiction Clinicians | 0 |
current estimates are that an estimated 1% of Americans suffer from a severe gambling problem. Including some 750,000 who are between ages 14 and 21.
Read More